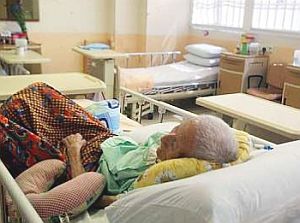
When our elderly relatives fall ill, we make all the decisions for them, thinking we know whats best for them. But are we really just putting our own interests, like financial considerations and convenience, ahead of theirs? Tee Shiao Eek explores the murky ethical dilemmas that arise when doctors and family members think they know whats best for elderly patients
The 78-year-old man lies unconscious on the hospital bed, hooked up to a breathing machine. His family stands at his bedside; the doctor, at the foot of the bed.
The atmosphere is awkward the doctor has suggested several treatment options, but the patients family members prefer to have their grandfather taken off the breathing machine.
Here, the doctor has to grapple with an ethical dilemma. His medical duty dictates that he provides the best treatment possible to save the patient. But seeing as the patient himself is unable to make the decision, should the doctor allow the familys wishes to override his expert opinion?
All healthcare workers face ethical dilemmas, but the practice of geriatric medicine is particularly complex, as with other vulnerable sub-groups like children and psychiatric patients, said Dr Chin Jing Jih of Singapores Tan Tock Seng Hospital, during the recent Asia-Pacific Geriatric Conference in Kuala Lumpur.
If youve ever tried convincing an elderly relative to let go of certain outdated beliefs, you will know how difficult it is to change the mindset of an older person.
Older people have a strong set of values, said Dr Chin, and it can influence a lot of the decisions they make, such as not wanting to take a certain medication because of its colour.
Family members and doctors need to bear in mind that an elderly patient is so much more vulnerable than an average person. They are physically weaker, and prone to psychological problems like depression. There are changes in their lives they may be struggling to come to terms with, like the gradual loss of a dominant position in the family.
There are also a lot of medically-related issues, such as multiple chronic illnesses and co-morbidities, said Dr Chin.
Any decision for the medical care of an elderly patient becomes mired in ethical complexities because more choices have to be made, treatment becomes more costly and the outcomes are uncertain.
Ethics, ethics
For the family members of the ailing grandfather, the decision to withdraw life-support would have been a difficult one, but perhaps it was driven by practical reasons.
Perhaps the elderly man had specified that he did not want to be on life support. Perhaps the family could not afford the cost of further treatment or hospitalisation fees.
Whatever the decision, it does not end here for the doctor. When he sees the next elderly patient, another ethical dilemma may arise, forcing him to make a choice between whats right and wrong morally, medically and legally.
Ethics is about the various options available and what are the reasons to support each choice, said Dr Chin. There are a lot of situations where there are no best options. It is the reason and relative weights placed on your options (that determine your decision).
When it comes to the health, life and death of an elderly patient, the most difficult ethical issues arise in situations that concern end-of-life care.
What is the extent of treatment to be provided? Should you withhold or withdraw medical treatment? How far do you go? If youre talking about quality of life, whose quality of life judgment is your decision based on? Dr Chin listed out some of the questions that doctors and family members would have to grapple with.
Palliative care is an important area of geriatric medicine, where the patients safety and well-being need to be balanced with his quality of life. For example, a doctor may ask himself, should opioids be used to relieve pain if it increases the risk of death, and compromises the decision-making capacity of the patient?
Another particularly contentious topic is right-to-die issues. Dr Chin pointed out that euthanasia, physician-assisted suicide or withdrawal of life-sustaining therapy are all different, and each need to be considered individually.
Advance care planning could prevent these ethical dilemmas from arising when your elderly relative is on her deathbed, but this is still trying to find a foothold in communities where it is taboo to talk about death or unpleasant eventualities, said Dr Chin
For example, could you bring yourself to ask your elderly mother whether she wishes to receive life-sustaining treatment if she becomes terminally ill?
In some elderly patients, such as those with dementia, other concerns further muddy the waters, such as decisions about whether to tube-feed or use restraints. Is it right to restrain an old lady to her bed, and justify it by saying that it prevents injuries?
Hes old, what does he know?
At a glance, its too easy to see that the elderly patient is usually the last one (if at all) to have a say in decisions about their health.
Most of the time, these patients are either incapacitated and unable to participate in any discussion, or are not given the opportunity to participate, said Dr Chin, elaborating that a lot of the time, the discussion is usually between the family and the doctor, bypassing the older patient.
In a lot of these ethical issues, the missing piece in the puzzle is always communication.
Sadly, nobody bothers to find out what the elderly patient really wants or thinks. He may want to know the results of his medical tests, but the doctor may collude with his family members to withhold the bad news.
He may not be given a choice in whether to receive or refuse medically beneficial treatment, such as surgery, because his family and doctor have made the decision for him instead. In fact, he may not even fully understand what is going on, because nobody has bothered to talk to him.
Filial society or not, the reality is that family members who make decisions on behalf of their elderly relatives may not have the patients best interests at heart.
There are many elderly patients who are deprived of valid medical treatment simply because their family has said no. Very often, when you ask the family what they are trying to achieve, the answer doesnt involve the patient, revealed Dr Chin. Instead, family members are more likely to point to financial constraints or the fact that there is no one at home to look after the patient.
Old dad has Alzheimers and wanders around unknowingly? Put restraints on him, say his children.
Dr Chin said frankly that this kind of response was an easy way out for family members, who tended to be more reactionary than constructive when faced with difficult issues.
But the blame is not to be placed squarely on family members and relatives alone. How often do doctors discuss issues with their elderly patients? Do doctors stop to consider that the patient is under a great deal of stress, is suffering from physical, cognitive or sensory impairment, is experiencing distressing symptoms, and is taking a lot of medications?
Sure, the doctor can rattle off statistics, but the patient may not be able to understand it, especially if he is hearing impaired, cannot see clearly or is in a lot of pain and discomfort.
When it comes to getting informed consent (or refusal) of treatment, the doctor should not demand for consent immediately, as a patient needs time to absorb a diagnosis and come to terms with it, said Dr Chin.
If a patient is sedated, the doctor should reduce the medication and then come back for a discussion when the patient is less sedated, he added.
Doctors and surgeons often make a common mistake: they only doubt the patients decision-making capacity if the patient disagrees with them.
However, Dr Chin pointed out that even if the patient agreed with the doctor, it might not be the right decision. Take, for example, the patient who agreed to let surgeons amputate his leg, because he thought that a new leg would grow out after the amputation.
A lot of the time, we dont question why the patient agrees with us, we only question their capacities when they disagree with us.
Who speaks for the patient?
What it comes to is an invisible tussle between doctors and family members, each wanting to make the decision for the elderly patient.
Who is the best person to make the decision? Is there even a best person?
With patients who are unable to make a decision, we frequently ask the family. But increasingly, we are realizing that the family may not necessarily be the best people to make that choice (or decision), said Dr Chin.
For someone who can provide a purely objective and professional point of view, we have to look to the doctor, to act as patient advocate.
However, this puts doctors in an ethical quandary, because they are torn between acting for the patient, and bowing to the judgment of family members who pay the medical bills.
Legally, there are provisions to eliminate this gray area, although many doctors themselves are not aware of it.
Under British common law, family consent is not valid consent (as opposed to Americas surrogate system). It is the professional who makes the decision for the incompetent patient, based on the patients best interests, explained Dr Chin.
This may relieve a doctor of the ethical dilemmas described above, but he is still held to the medical code of ethics to provide the best care for his patient.
Treatment has to be looked upon in perspective of the patients quality of life and other factors, including medical factors, pre-morbid conditions, personal values, societal norms, legal obligations and economic concerns, said Dr Chin.
He cautioned doctors against practicing arbitrary bedside rationing, where they make decisions based on personal reasons or who is more/less likely to sue.
Copyright © Global Action on Aging
Terms of Use |
Privacy Policy | Contact
Us



