For the Very Old, a Surprise in Blood
Pressure Readings
By Paula Span, The New
York Times
August 8, 2012
World
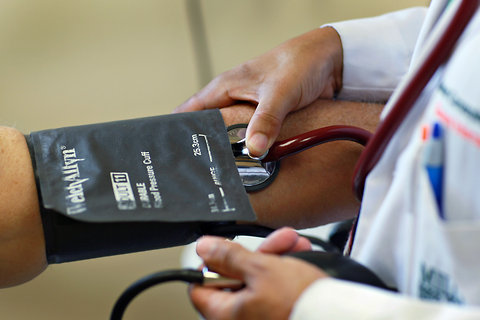 Image
Credit: Joe Raedle/Getty Images
Image
Credit: Joe Raedle/Getty Images
It’s such a routine thing: A
nurse wraps the cuff around your elderly
relative’s arm, squeezes the bulb, listens with
a stethoscope and says: “120 over 60. Very
good.” Smiles all around (this was my
89-year-old father’s latest reading), because
everyone knows that high blood pressure is a
risky proposition.
Or is it? Reading a study and an editorial just
published in Archives of Internal Medicine, I
was startled to learn that in the very elderly —
those over 85, say — high blood pressure may
indicate better health while lower numbers could
mean trouble ahead. For a layperson, this was
such a through-the-looking-glass moment that I
called Dr. James Goodwin, a geriatrician at the
University of Texas Medical Branch in Galveston
who wrote the editorial, and asked, in essence,
does everyone know this but me?
“These are very well-kept secrets,” he said.
“That high blood pressure in those over 85
predicts longer survival would probably be news
to 95 percent of practicing physicians.” Which
was not entirely reassuring.
Dr. Goodwin has been writing for years about the
way blood pressure readings and other indicators
of health, like weight and cholesterol, take on
different meanings in advanced age. What sparked
this latest discussion was a new study, bluntly
titled “Rethinking the Association of High Blood
Pressure With Mortality in Elderly Adults,” that
examined whether walking speed might identify
which older people are more at risk from high
blood pressure, as hypertension is commonly
known.
An Oregon State University epidemiologist,
Michelle Odden, and a team at the University of
California, San Francisco, reviewed data from
the National Health and Nutrition Examination
Survey, following 2,340 people over age 65 for
an average of five years. The researchers
divided the participants into categories based
on the pace at which they walked a 20-foot
corridor. Among fast walkers, who averaged a
pace of 1.8 miles per hour or better, those with
elevated blood pressure had a 35 percent higher
risk of dying — the same risk seen in younger
adults. But in slower walkers, hypertension did
not increase mortality.
And in a small group of participants who didn’t
complete the walk, those with high blood
pressure had a 60 percent lower risk of death.
If these were the only data suggesting that
hypertension’s effects begin to reverse in old
age, we could shrug them off. In this study,
those who didn’t or couldn’t walk 20 feet
offered a variety of reasons: many had physical
limitations or felt unsafe, but “some just
showed up late for their appointments,” Dr.
Odden acknowledged. Hard to draw conclusions
from that.
But this isn’t the first study showing an
inverse association — hypertension equals longer
life — in the very old. “It expands on a fairly
substantial amount of research on the
relationship between blood pressure and
survival,” Dr. Goodwin said. What doctors should
do about hypertension in the very elderly –
treat it or leave it alone? – has generated
controversy for decades, particularly since
clinical drug trials often exclude the elderly,
leaving doctors with scant evidence to go on.
The medical guidelines for treating
hypertension, set by a Joint National Committee
in 2003 (and about to be updated) established a
goal of 140/90; the systolic reading, the first
of the two numbers, is the more important
measure in people over age 50. The guidelines
recommend medication for people who have higher
blood pressure (as more than two-thirds of those
over age 65 do) because of the well-established
risk of heart attack and stroke. The
recommendations don’t differ for the very old,
but perhaps they should.
“The paradigm in medicine is, high blood
pressure is bad, treating it is good,” Dr. Odden
said. “We’re saying, maybe we need to look more
closely at the guidelines and tailor them more
to older adults.” Her study shows that “it’s not
just age, it’s your physiology, your functional
status, frailty” that matters.
What do we do with this? For younger people, the
decisions are clear-cut: Reducing high blood
pressure is a priority, and our increasing
success at it represents a major public health
victory, one reason we’ve become an aging
nation.
In the very old, however, lower readings could
mean good health, or they might also indicate
that a patient’s heart isn’t pumping
efficiently, while higher readings may mean
robustness. “It can make you quite a bit less
aggressive in treatment,” Dr. Goodwin said,
especially since hypertension drugs can cause
falls and dizziness.
Dr. Ken Covinsky, a geriatrician at the
University of California, San Francisco, and
senior author of the new study, said he’d
probably recommend treatment for an 80-year-old
tennis player with high blood pressure, but
would be less worried about a frail 80-year-old
with a systolic reading of 160, especially if
she was already prone to falling.
“Do we really want to give her a ninth
medication?” he asked. “I’d feel a little queasy
about that.”
It’s a conversation worth having with a doctor,
though hypertension treatment has become so
reflexive that it could be a tough discussion.
“Few physicians are aware of these findings, and
they’re going to be suspicious,” Dr. Goodwin
said.
But give it a try anyway, he said: “We have to
bring the complexity of decision making in the
elderly into the light of day.”
|



